
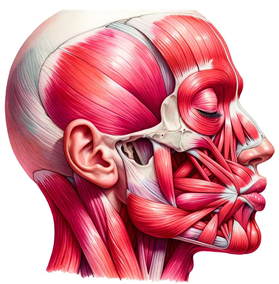
This paper delves deeply into the innovative realm of integrating human emotions with wearable technology. The primary focus is on the conceptualization and development of a kiss transfer device that harnesses the power of wearable technology to bridge the physical gap in human-human interactions. By investigating the intricate nuances of the human-human kissing process, the research seeks to replicate this intimate gesture through a technological medium. The paper not only elaborates on the anatomy, evolution, and hormonal dynamics of kissing but also underscores the transformative potential of wearable technology in capturing and transmitting these intimate moments. This exploration opens up new horizons for long-distance relationships, offering a tangible touchpoint that goes beyond traditional communication methods. Through this pioneering work, the research positions wearable technology as not just a tool for communication but as an extension of our human emotions and expressions.
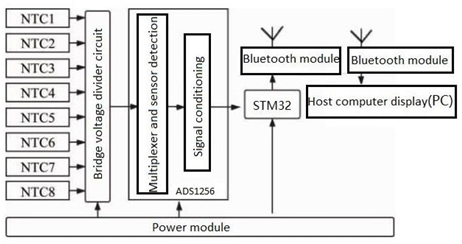
Application prospects for wearable body surface microfluidic system in sports
Vol 3, Issue 1, 2022
Download PDF
Abstract
The wearable body surface microfluidic system has great application potential in the field of sports. The use of the wearable body surface microfluidic system to monitor the physiological state of athletes can solve problems faced such as long inspection cycle in sports monitoring, difficulties in continuous monitoring, dependence on laboratory platforms, athlete resistance and other problems faced in technological integration to promote the development of the sports field. In recent years, the development of key technologies such as microfluidic chips and microneedle delivery provides an ideal solution for real-time monitoring and even immediate intervention of physiological states during exercise. This paper summarizes the latest research progress of wearable body surface microfluidic systems and focuses on eight wearable body surface microfluidic systems that may be applied in the field of sports, with their application prospects in sports analyzed and discussed. Finally, the application direction of the wearable body surface microfluidic system that may achieve breakthroughs is illustrated with the prospect demonstration of the future research and development direction of wearable sports equipment. This paper aims to focus on technical problems in the development of the sports field, provide multi-disciplinary solutions and advocate technology integration as well as provide scientific and technological assistance for the development of the sports field.
Keywords
References
- Lee BC, Chen S, Sienko KH. A wearable device for real-time motion error detection and vibrotactile instructional cuing. IEEE Transactions on Neural Systems and Rehabilitation Engineering 2011; 19(4): 374–381.
- Villa F, Magnani A, Maggioni MA, et al. Wearable multi-frequency and multi-segment bioelectrical impedance spectroscopy for unobtrusively tracking body fluid shifts during physical activity in real-field applications: A preliminary study. Sensors 2016; 16(5): 673.
- Maier D, Laubender E, Basavanna A, et al. Toward continuous monitoring of breath biochemistry: A paper-based wearable sensor for real-time hydrogen peroxide measurement in simulated breath. ACS Sensors 2019; 4(11): 2945–2951.
- Feng S, Caire R, Cortazar B, et al. Immunochromatographic diagnostic test analysis using Google Glass. ACS Nano 2014; 8(3): 3069–3079.
- Liu Y, Pharr M, Salvatore GA. Lab-on-skin: A review of flexible and stretchable electronics for wearable health monitoring. ACS Nano 2017; 11(10): 9614–9635.
- Heikenfeld J, Jajack A, Rogers J, et al. Wearable sensors: Modalities, challenges, and prospects. Lab on a Chip 2018; 18(2): 217–248.
- Koh A, Kang D, Xue Y, et al. A soft, wearable microfluidic device for the capture, storage, and colorimetric sensing of sweat. Science Translational Medicine 2016; 366(8): 165.
- Choi J, Xue Y, Xia W, et al. Soft, skin-mounted microfluidic systems for measuring secretory fluidic pressures generated at the surface of the skin by eccrine sweat glands. Lab on a Chip 2017; 17(15): 2572–2580.
- Sekine Y, Kim SB, Zhang Y, et al. A fluorometric skin-interfaced microfluidic device and smartphone imaging module for in situ quantitative analysis of sweat chemistry. Lab on a Chip 2018; 18(15): 2178–2186.
- Zhang Y, Guo H, Kim SB, et al. Passive sweat collection and colorimetric analysis of biomarkers relevant to kidney disorders using a soft microfluidic system. Lab on a Chip 2019; 19(9): 1545–1555.
- Choi J, Kang D, Han S, et al. Thin, soft, skin-mounted microfluidic networks with capillary bursting valves for chrono-sampling of sweat. Advanced Healthcare Materials 2017; 6(5): 1601355.
- Bandodkar AJ, Gutruf P, Choi J, et al. Battery-free, skin-interfaced microfluidic/electronic systems for simultaneous electrochemical, colorimetric, and volumetric analysis of sweat. Science Advances 2019; 5(1).
- Kim SB, Lee KH, Raj MS, et al. Soft, skin-interfaced microfluidic systems with wireless, battery-free electronics for digital, real-time tracking of sweat loss and electrolyte composition. Small 2018; 14(45): 1802876.
- Kim SB, Zhang Y, Won SM, et al. Super-absorbent polymer valves and colorimetric chemistries for time-sequenced discrete sampling and chloride analysis of sweat via skin-mounted soft microfluidics. Small 2018; 14(12): 1703334.
- Gowers SAN, Freeman DME, Rawson TM, et al. Development of a minimally invasive microneedle-based sensor for continuous monitoring of β-lactam antibiotic concentrations in vivo. ACS Sensors 2019; 4(4): 1072–1080.
- Lee H, Choi TK, Lee YB, et al. A graphene-based electrochemical device with thermos-responsive microneedles for diabetes monitoring and therapy. Nature Nanotechnology 2016; 11(6): 566–572.
- Li W, Tang J, Terry RN, et al. Long-acting reversible contraception by effervescent microneedle patch. Science Advances 2019; 5(11): eaaw8145.
- Di J, Yao S, Ye Y, et al. Stretch-triggered drug delivery from wearable elastomer films containing therapeutic depots. ACS Nano 2015; 9(9): 9407–9415.
- Goodwin ML, Harris JE, Hernández A, et al. Blood lactate measurements and analysis during exercise: A guide for clinicians. Journal of Diabetes Science and Technology 2007; 1(4): 558–569.
- Reeder JT, Choi J, Xue Y, et al. Waterproof, electronics-enabled, epidermal microfluidic devices for sweat collection, biomarker analysis, and thermography in aquatic settings. Science Advances 2019; 5(1): eaau6356.
- Ray T, Choi J, Reeder J, et al. Soft, skin-interfaced wearable systems for sports science and analytics. Current Opinion in Biomedical Engineering 2019; 9: 47–56.
- Alizadeh A, Burns A, Lenigk R, et al. A wearable patch for continuous monitoring of sweat electrolytes during exertion. Lab on a Chip 2018; 18(17): 2632–2641.
- Gao W, Emaminejad S, Nyein HYY, et al. Fully integrated wearable sensor arrays for multiplexed in situ perspiration analysis. Nature 2016; 529(7587): 509–514.
- Choi J, Ghaffari R, Baker LB, et al. Skin-interfaced systems for sweat collection and analytics. Science Advances 2018; 4(2): eaar3921.
- Emaminejad S, Gao W, Wu E, et al. Autonomous sweat extraction and analysis applied to cystic fibrosis and glucose monitoring using a fully integrated wearable platform. Proceedings of the National Academy of Sciences 2017; 114(18): 4625–4630.
- Choi J, Bandodkar AJ, Reeder JT, et al. Soft, skin-integrated multifunctional microfluidic systems for accurate colorimetric analysis of sweat biomarkers and temperature. ACS Sensors 2019; 4(2): 379–388.
- Buono MJ, Lee NVL, Miller PW. The relationship between exercise intensity and the sweat lactate excretion rate. The Journal of Physiological Sciences 2010; 60(2): 103–107.
- Moyer J, Wilson D, Finkelshtein I, et al. Correlation between sweat glucose and blood glucose in subjects with diabetes. Diabetes Technology & Therapeutics 2012; 14(5): 398–402.
- Kim J, Campbell AS, Wang J. Wearable non-invasive epidermal glucose sensors: A review. Talanta 2018; 177: 163–170.
- Kim YC, Park JH, Prausnitz MR. Microneedles for drug and vaccine delivery. Advanced Drug Delivery Reviews 2012; 64(14): 1547–1568.
- Wang M, Hu L, Xu C. Recent advances in the design of polymeric microneedles for transdermal drug delivery and biosensing. Lab on a Chip 2017; 17(8): 1373–1387.
- Petchakup C, Tay HM, Li KHH, et al. Integrated inertial-impedance cytometry for rapid label-free leukocyte isolation and profiling of neutrophil extracellular traps (NETs). Lab on a Chip 2019; 19(10): 1736–1746.
- Sharma A, Smyrk TC, Levy MJ, et al. Fasting blood glucose levels provide estimate of duration and progression of pancreatic cancer before diagnosis. Gastroenterology 2018; 155(2): 490–500.
- Babity S, Roohnikan M, Brambilla D. Advances in the design of transdermal microneedles for diagnostic and monitoring applications. Small 2018; 14(49): 1803186.
- Fukushima K, Ise A, Morita H, et al. Two-layered dissolving microneedles for percutaneous delivery of peptide/protein drugs in rats. Pharmaceutical Research 2011; 28(1): 7–21.
- Yang J, Liu X, Fu Y, et al. Recent advances of microneedles for biomedical applications: drug delivery and beyond. Acta Pharmaceutica Sinica B 2019; 9(3): 469–483.
- Wang P, Cornwell M, Prausnitz MR. Minimally invasive extraction of dermal interstitial fluid for glucose monitoring using microneedles. Diabetes Technology & Therapeutics 2005; 7(1): 131–141.
- Bariya SH, Gohel MC, Mehta TA, et al. Microneedles: An emerging transdermal drug delivery system. Journal of Pharmacy and Pharmacology 2012; 64(1): 11–29.
- Tasca F, Tortolini C, Bollella P, et al. Microneedle-based electrochemical devices for transdermal biosensing: A review. Current Opinion in Electrochemistry 2019; 16: 42–49.
- Rawson TM, Gowers SAN, Freeman DM E, et al. Microneedle biosensors for real-time, minimally invasive drug monitoring of phenoxymethylpenicillin: A first-in-human evaluation in healthy volunteers. The Lancet Digital Health 2019; 1(7): e335–e343.
Supporting Agencies
Copyright (c) 2022 Shengtai Bian, Shun Ye, Shufei Yang

This work is licensed under a Creative Commons Attribution 4.0 International License.

Prof. Zhen Cao
College of Information Science & Electronic Engineering, Zhejiang University
China, China
Processing Speed
-
-
-
- <5 days from submission to initial review decision;
- 62% acceptance rate
-
-
Asia Pacific Academy of Science Pte. Ltd. (APACSCI) specializes in international journal publishing. APACSCI adopts the open access publishing model and provides an important communication bridge for academic groups whose interest fields include engineering, technology, medicine, computer, mathematics, agriculture and forestry, and environment.





