
Asia Pacific Academy of Science Pte. Ltd. (APACSCI) specializes in international journal publishing. APACSCI adopts the open access publishing model and provides an important communication bridge for academic groups whose interest fields include engineering, technology, medicine, computer, mathematics, agriculture and forestry, and environment.
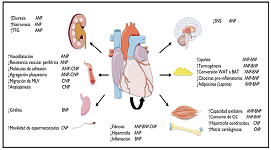
Coronavirus and cardiovascular system
Vol 2, Issue 2, 2021
Download PDF
Abstract
The current pandemic caused by the new coronavirus (SARS-CoV-2) has been the focus of worldwide health concern since its appearance. Its high transmissibility associated with the absence of an effective treatment implies a hard impact in the research area. Reports on atypical forms of presentation, associated risk factors and drugs tested to reduce morbidity and mortality saturate the media. The cardiological community is actively involved, since cardiovascular manifestations are frequent and varied, and an increased risk of poor outcome has been observed in individuals with previous cardiovascular disease. The aim of the review is to provide the available evidence on this topic, with the caveat that the information is dynamic.
Keywords
References
- Driggin E, Madhavan MV, Bikdeli B, et al. Cardiovascular Considerations for Patients, Health Care Workers, and Health Systems During the Coronavirus Disease 2019 (COVID-19) Pandemic. J Am Coll Cardiol. 2020. doi: 10.1016/j. jacc.2020.03.031
- Case viewer. Available online: https://www.gub.uy/sis- tema-nacional-emergencias/ (accessed on 24 April 2021).
- Fried JA, Ramasubbu K, Bhatt R, et al. The Variety of Cardiovascular Presentations of COVID-19. Circulation. 2020; 141(23): 1930-1936. doi: 10.1161/circulationaha.120.047164
- Tan W, Aboulhosn J. The cardiovascular burden of coronavirus disease 2019 (COVID-19) with a focus on congenital heart disease. International Journal of Cardiology. 2020; 309: 70-77. doi: 10.1016/j.ijcard.2020.03.063
- Cascella M, Rajnik M, Cuomo A, et al. Features, evaluation and treatment coronavirus (COVID-19). Available online: https://www.ncbi.nlm.nih.gov/books/NBK554776/ (accessed on 24 April 2021).
- Akhmerov A, Marbán E. COVID-19 and the Heart. Circulation Research. 2020; 126(10): 1443-1455. doi: 10.1161/circresaha.120.317055
- Zhou F, Yu T, Du R, et al. Clinical course and risk factorsfor mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020; 395(10229): 1054-1062. doi: 10.1016/S0140-6736(20) 30566-3
- Wang D, Hu B, Hu C, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020. doi: 10.1001/ jama.2020.1585
- Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020; 395(10223): 497-506. doi: 10.1016/S0140-6736(20)30183-5
- Shi S, Qin M, Shen B, et al. Association of Cardiac Injury with Mortality in Hospitalized Patients With COVID-19 in Wuhan, China. JAMA. 2020. doi: 10.1001/jamacar- dio.2020.0950
- Wu Z, McGoogan JM. Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China. JAMA. 2020; 323(13): 1239. doi: 10.1001/jama.2020.2648
- Libby P, Ridker PM, Hansson GK. Inflammation in Atherosclerosis. Journal of the American College of Cardiology. 2009; 54(23): 2129-2138. doi: 10.1016/j.jacc.2009.09.009
- Zheng YY, Ma YT, Zhang JY, et al. COVID-19 and the cardiovascular system. Nature Reviews Cardiology. 2020; 17(5): 259-260. doi: 10.1038/s41569-020-0360-5
- McMurray J, Pfeffer M, Solomon S. Renin-angio-angio- tensin-aldosterone system inhibitors in patients with COVID-19. N Engl J Med. 2020; 382(17). doi: 10. 1056/NEJMsr2005760
- Zhang P, Zhu L, Cai J, et al. Association of inpatient use of angiotensin converting enzyme inhibitors and Angiotensin II receptor blockers with mortality among patients with hypertension hospitalized with COVID-19. Circ Res. 2020; 127(6): e147. doi: 10.1161/RES.0000000000000434
- Frankie Tam C, Cheung K, Lam S, et al. Impact of Coronavirus Disease 2019 (COVID-19) Outbreak on ST-Segment–Elevation Myocardial Infarction Care in Hong Kong, China. Circulation: Cardiovascular Quality and Outcomes. 2020; 13(4). doi: 10.1161/circoutcomes.120.006631
- Alhogbani T. Acute myocarditis associated with novel Middle east respiratory syndrome coronavirus. Ann Saudi Med. 2016; 36(1): 78-80. doi: 10.5144/ 0256-4947.2016.78
- Zeng JH, Liu YX, Yuan J, et al. First Case of COVID-19 Infection with Fulminant Myocarditis Complication: Case Report and Insights. Published online March 11, 2020. doi: 10.20944/preprints202003.0180.v1
- Xiong TY, Redwood S, Prendergast B, et al. Coronaviruses and the cardiovascular system: acute and long-term implications. European Heart Journal. 2020; 41(19): 1798-1800. doi: 10.1093/eurheartj/ehaa231
- Bangalore S, Sharma A, Slotwiner A, et al. ST-Segment Elevation in Patients with Covid-19—A Case Series. New England Journal of Medicine. 2020; 382(25): 2478-2480. doi: 10.1056/nejmc2009020
- Romaguera R, Cruz-González I, Jurado-Román A, et al. Considerations on the invasive approach to ischemic and structural heart disease during the COVID-19 coronavirus outbreak. Consensus document of the Association of Interventional Cardiology and the Association of Ischemic Heart Disease and Acute Cardiovascular Care of the Spanish Society of Cardiology. REC Interv Cardiol. 2020. doi: 10.24875/RECIC.M20000119
- Mahmud E, Dauerman HL, Welt FGP, et al. Management of acute myocardial infarction during the COVID-19 pandemic. J Am Coll Cardiol. 2020. doi: 10.1016/j. jacc.2020.04.039
- Lazzerini P, Boutjdir M, Capecchi PL. COVID-19, arrhythmic risk and inflammation: Mind the Gap! Circulation. 2020. doi: 10.1161/CIRCULA-TIONAHA.120.047293
- Vidovich MI. Transient Brugada-Like Electrocardiographic Pattern in a Patient With COVID-19. JACC: Case Reports. 2020; 2(9): 1245-1249. doi: 10.1016/j.jaccas.2020.04.007
- Lazzerini PE, Capecchi PL, Laghi-Pasini F. Systemic inflammation and arrhythmic risk: lessons from rheumatoid arthritis. European Heart Journal. Published online June 1, 2016: ehw208. doi: 10.1093/eurheartj/ehw208
- Bikdeli B, Madhavan MV, Jimenez D, et al. COVID-19 and thrombotic or thromboembolic disease: implications for prevention, antithrombotic therapy, and Follow-up. J Am Coll Cardiol. 2020. doi: 10.1016/j.jacc. 2020.04.031
- Ciceri F, Beretta L, Scandroglio AM, et al. Microvascular COVID-19 lung vessels obstructive thromboinflammatory syndrome (MicroCLOTS): an atypical acute respiratory distress syndrome working hypothesis. Critical Care and Resuscitation. 2020; 22(2): 95-97. doi: 10.51893/2020.2.pov2
- Helms J, Tacquard C, Severac F, et al. High risk of thrombosis in patients in severe SARS-CoV-2 infection: a multicenter prospective cohort study. Intensive Care Med. 2020. doi: 10.1007/s00134-020- 06062-x
Supporting Agencies
Copyright (c) 2021 Dres Sofía Noria, Juan Pablo Bachini, María Victoria Ramos

This work is licensed under a Creative Commons Attribution 4.0 International License.

This site is licensed under a Creative Commons Attribution 4.0 International License (CC BY 4.0).

Prof. Prakash Deedwania
University of California,
San Francisco, United States




